- Monday and Wednesday 10am to 7pm (Additional appointment times available upon request)
A woman’s body goes through many transitions in a lifetime with many of the physical changes affected by hormones, lifestyle, and social environment. The pelvic floor as an essential part of the body and is also sensitive to these changes and requires attention and care so that it can continue support the body.
Pregnancy places significant physical stress on your body, especially the pelvic floor. Managing these changes can feel overwhelming. At Shireen Sundrani Physiotherapy Services, we support you throughout your motherhood journey, from prenatal care to helping you recover quickly postpartum

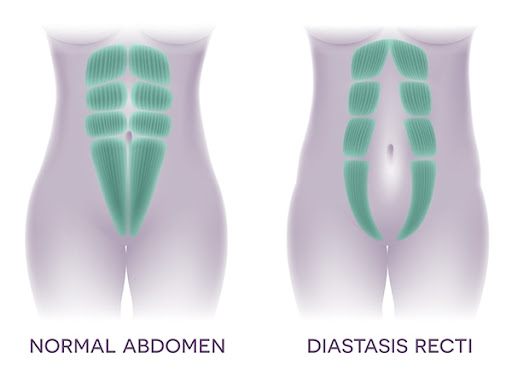
DRA occurs when the two rectus abdominis muscles separate more than usual, causing the linea alba to thin and widen. Signs during pregnancy may include doming, coning, or bulging of the belly when lifting your head, carrying heavy objects, or exercising.
Although DRA is a normal part of pregnancy, it’s important to address the resulting muscle imbalances to maintain comfort during pregnancy and promote smooth postpartum recovery.
The growing baby places pressure on your pelvic floor, which may lead to bladder problems:

The pelvic girdle includes the pelvis, excluding the sacrum and tailbone. PGP can cause pain in the front (symphysis pubis/groin) or back (sacroiliac joints) of the pelvis.
Early diagnosis and treatment are safe at any stage of pregnancy or postpartum and can help relieve pain, improve mobility, and enhance quality of life

Preparing for birth can feel overwhelming, but your pelvic floor plays a vital role during delivery. At Shireen Sundrani Physiotherapy Services, we guide you through:

The fourth trimester and beyond is often one of the most challenging times for new moms. Balancing the demands of caring for your baby while healing your body can feel overwhelming. At Shireen Sundrani Physiotherapy Services, we understand these challenges and are dedicated to supporting you throughout your postpartum recovery, helping you regain strength, mobility, and confidence.

Women who deliver vaginally are two to three times more likely to experience stress incontinence compared to those who have never given birth. Factors such as perineal tearing or an episiotomy can affect pelvic floor strength and lead to bladder problems.
Some women may also experience poor bowel control or accidental passing of gas. The good news is that all of these issues can be improved or reversed with specialized pelvic physiotherapy, helping you regain control and confidence in your daily life.

Women who deliver vaginally are two to three times more likely to experience stress incontinence compared to those who have never given birth. Factors such as perineal tearing or an episiotomy can affect pelvic floor strength and lead to bladder problems.
Some women may also experience poor bowel control or accidental passing of gas. The good news is that all of these issues can be improved or reversed with specialized pelvic physiotherapy, helping you regain control and confidence in your daily life.

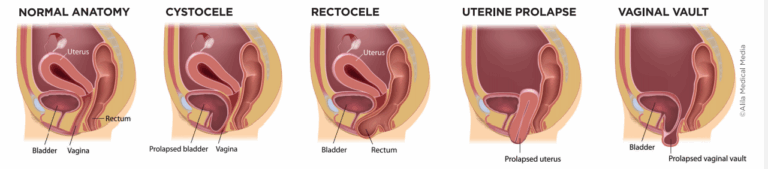
Pelvic organ prolapse occurs when one or more vaginal compartments descend due to weakened pelvic floor support. Women often notice a bulging or heaviness sensation. POP is common, affecting more than half of adult women.
Mild to moderate prolapse responds well to pelvic physiotherapy, and with proper guidance, you can safely return to your physical activities.
Approximately one-third of women report persistent pain during intercourse up to 18 months postpartum. Pelvic floor stress or injury can cause tension, leading to aching or burning sensations.
If you are breastfeeding, low estrogen levels may also cause vaginal dryness. At Shireen Sundrani Physiotherapy Services, we address all contributing factors to help you regain comfort and confidence in your sex life.

Proper care of scars from Cesarean delivery, perineal tearing, or episiotomy can prevent adhesions and restricted mobility. Scar restrictions can affect pelvic floor function, core strength recovery, and sexual activity. Our targeted scar therapy promotes healing and restores mobility.

Motherhood places unique demands on your body. Along with core strengthening, we help relieve low back pain, neck and shoulder tension, wrist discomfort, and thumb strain caused by daily caregiving. Our goal is to help you enjoy motherhood, pain-free.

If you are experiencing pelvic pain, you are not alone. Around 20% of women will experience pelvic pain at some point in their lives. The causes can be complex and varied, which can feel overwhelming. At Shireen Sundrani Physiotherapy Services, we are committed to helping you navigate your healing journey with individualized care and support.

The vulva is the external part of your genitals, including the mons pubis, vaginal opening, labia majora and minora, clitoris, and perineum. Vulvodynia is persistent discomfort in the vulva lasting three months or longer, not caused by infection, skin disorder, or other medical conditions.
Symptoms may include:
Causes often involve tension in the pelvic floor muscles and surrounding tissues.
The vestibule is the area surrounding the urethral and vaginal openings, hymenal tags, and inner edges of the labia minora. It contains the Bartholin’s gland (for lubrication) and small vestibule glands (for vaginal discharge).
Vestibulodynia is pain localized to this sensitive area, often triggered by:
Pain is typically described as burning, stinging, or cutting, sometimes felt deeper in the vagina.

Vaginismus is the involuntary contraction or spasm of the pelvic floor muscles during any attempted vaginal penetration, such as intercourse or speculum insertion, often due to fear of pain.
It can develop due to:
At Shireen Sundrani Physiotherapy Services, we address both the physical and emotional components of vaginismus, creating a safe and supportive path to recovery.

The coccyx, or tailbone, is a small but important bone that serves as the attachment point for multiple muscles, ligaments, and tendons. Along with the sitting bones, it provides weight-bearing support while sitting.
Coccydynia is characterized by a dull, achy pain at the tip of the tailbone, often felt between the buttocks. Tenderness may be noticed with touch or prolonged sitting, standing, or lying down. Causes can include falls or prolonged pushing during childbirth in the lithotomy position.
Pelvic physiotherapy can effectively treat tailbone pain, restoring comfort and mobility.
Pelvic floor dysfunction often coexists with complex conditions such as:
Interstitial Cystitis (IC) / Painful Bladder Syndrome (PBS)
Endometriosis
Irritable Bowel Syndrome (IBS)
Lichen Sclerosus (LS)
Ehlers-Danlos Syndrome (EDS)
The organs involved in these conditions are closely connected with the pelvic floor muscles, ligaments, and surrounding tissues. Addressing pelvic floor imbalance is an essential part of managing these conditions, and it is supported by current medical research.
At Shireen Sundrani Physiotherapy Services, we provide one-on-one care including hands-on internal and external therapy, guided self-care programs, and collaboration with your healthcare team for a multidisciplinary approach.
Patients with IC/PBS often experience bladder and pelvic pain, urinary urgency, frequency, and burning. Hypertonic or tight pelvic floor and pelvic girdle muscles (e.g., hip adductors, abdominals) can mimic these symptoms.
Pelvic physiotherapy can reduce or eliminate these debilitating symptoms and restore bladder function.
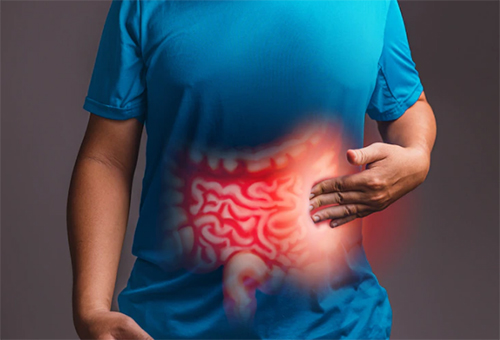
Symptoms of endometriosis include painful cramping, painful intercourse, bladder or bowel discomfort, and infertility. Inflammation can affect the pelvic and abdominal organs, muscles, and fascia, leading to dysfunction.
Treatment may include:

IBS can cause abdominal pain, bloating, gas, constipation, diarrhea, or both, which may lead to pelvic floor dysfunction such as:
Pelvic physiotherapy can restore bowel control and relieve pelvic floor dysfunction.
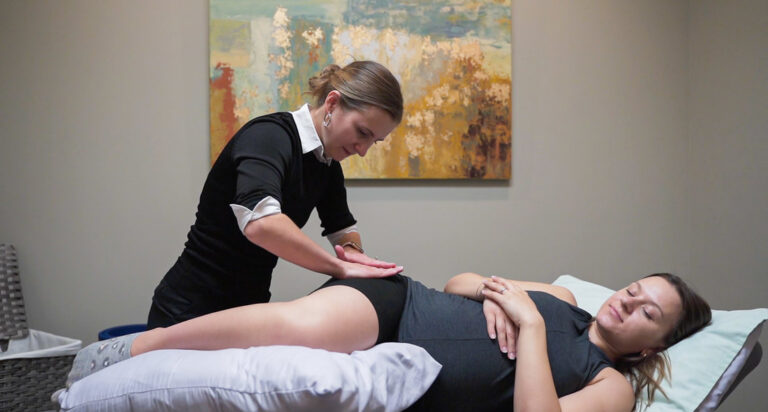
LS is a chronic inflammatory condition affecting the vulvar and anal areas, causing itching, painful intercourse, and painful urination. Scar tissue can lead to fusion of the labia minora and narrowing of the vaginal opening.
Pelvic physiotherapy targets the underlying muscular impairments to reduce pain and restore function.
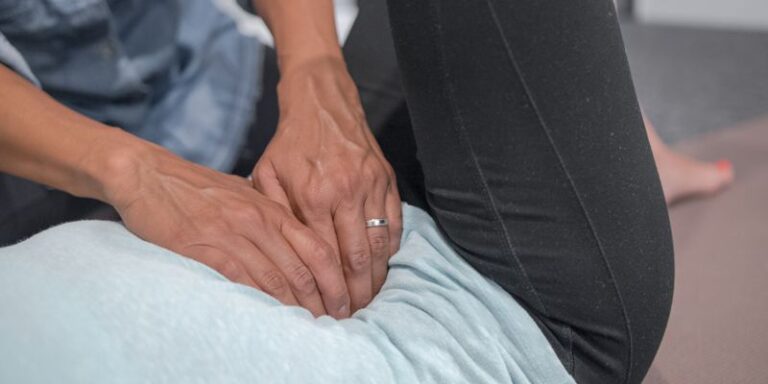
EDS is a connective tissue disorder that affects skin, ligaments, tendons, blood vessels, and pelvic organs. People with EDS may experience:
Pelvic physiotherapy helps reinforce pelvic stability, improve bladder function, and manage POP and pelvic pain.

Contact us today for a holistic assessment and treatment of your pelvic floor and a tailored treatment plan.
Your Partner in Recovery.
Offering advanced, personalized physiotherapy services focused on restoring mobility and accelerating your return to full health.
Monday and Wednesday
10 am to 7 pm (Additional appointment times available upon request)